LUMBAR SPINE & SLIP DISC (HERNIATED DISC)
UNDERSTANDING THE CONDITION
The vertebral column, also called the spinal column or backbone, is made up of 33 bones known as vertebrae. Each vertebra is separated by intervertebral discs, which are strong yet flexible cushions that absorb shock and allow movement.
These discs, along with ligaments and facet joints, help maintain the spine’s alignment, stability, and flexibility, making everyday movements like bending and twisting possible.
The lumbar spine (lower back) usually consists of five vertebrae and carries most of the body’s weight. Because of its mobility and load-bearing function, the lumbar spine is more prone to conditions like:
Lumbar slip disc (herniated disc)
Spinal stenosis
Degenerative disc disease
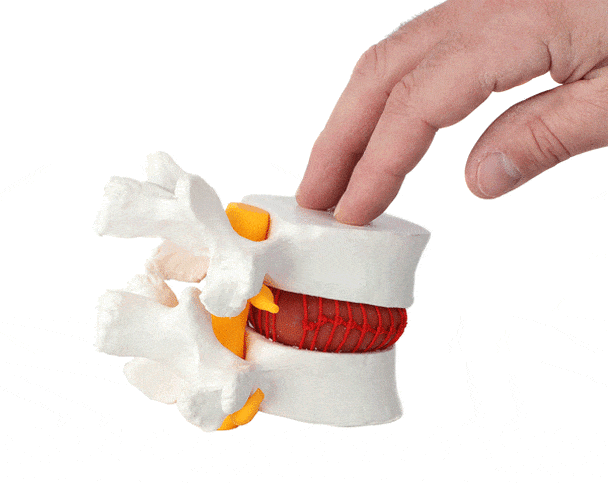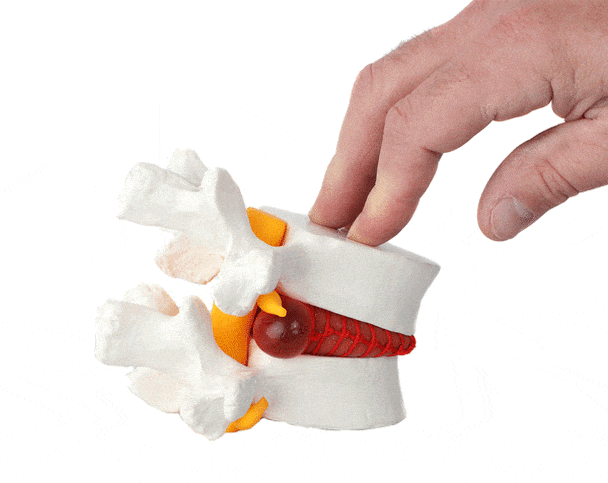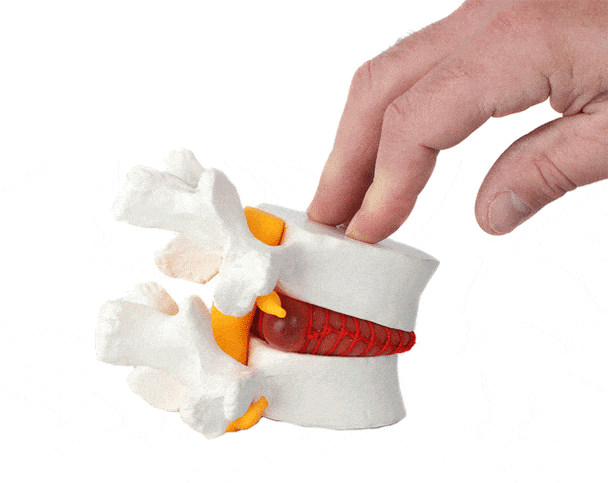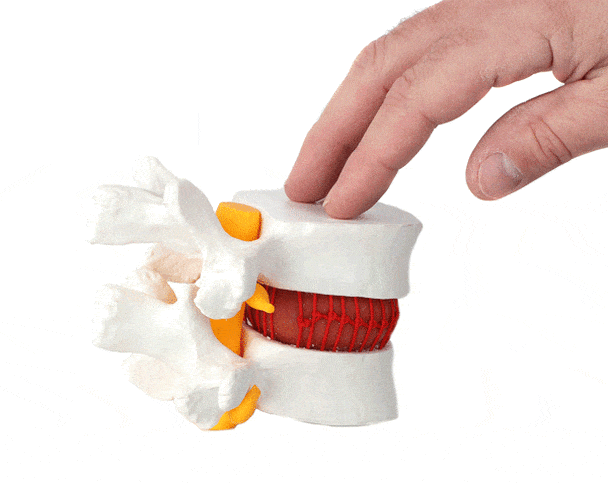

WHAT IS A LUMBAR SLIP DISC (HERNIATED DISC)?
A lumbar herniated disc, commonly called a slip disc, occurs when:
The outer fibrous layer of the disc (annulus fibrosus) tears
The inner gel-like core (nucleus pulposus) pushes out
This bulge compresses nearby spinal nerves
SYMPTOMS OF
LUMBAR SLIP DISC
A lumbar herniated disc can cause:
Intermittent or continuous lower back pain
Pain that worsens with movement, coughing, sneezing, or prolonged standing
Muscle spasms in the lower back
Sciatica – pain radiating from the back or buttock down the leg to the calf or foot
Muscle weakness in the legs
Numbness or tingling in the leg or foot
Difficulty in walking
Changes in bladder or bowel function (in severe cases)
When a nerve is compressed, it leads to a pinched nerve, causing symptoms such as pain, numbness, tingling, or weakness in the legs, often referred to as sciatica.
Note: These symptoms may overlap with other spine conditions. A proper medical diagnosis is essential.


CAUSES & RISK FACTORS OF SLIP DISC
Degenerative changes
(most common cause)
As part of aging:
Intervertebral discs lose water content
Discs become less flexible
Increased risk of tears and herniation
WHO IS AT RISK?
The most commonly affected age group is 25 to 40 years, where early degeneration begins but activity levels remain high.
High-risk profiles include:
Sedentary individuals with occasional strenuous activity
Overweight or obese individuals
People with poor posture or prolonged sitting habits
Individuals involved in heavy physical work or intense activity
This can cause a tear in the annulus fibrosus, allowing the nucleus pulposus to herniate into the spinal canal.
Note: These symptoms may overlap with other spine conditions. A proper medical diagnosis is essential.
Acute injury or strain
Slip disc can also occur in younger individuals due to:
Injury or trauma
Sudden twisting movements
Heavy lifting


TESTS & DIAGNOSIS FOR LUMBAR DISC PROBLEMS
If symptoms of slip disc are present, the following tests may be advised:
MRI (Magnetic Resonance Imaging):
The best diagnostic tool to evaluate spinal cord, nerves, discs, and ligamentsEMG (Electromyography):
Assesses nerve function and helps identify the exact cause of pain
TREATMENT OF LUMBAR SLIP DISC
IS SURGERY ALWAYS REQUIRED?
No. Most slip disc cases can be treated without surgery.
Non-surgical (Conservative) Treatment:
Rest (short-term, controlled)
Medications to reduce inflammation and pain
Muscle relaxants
Epidural steroid injections or nerve blocks
Since symptoms can mimic other spine conditions, additional tests may be required for accurate diagnosis.
Complete rest reduces pressure on the disc, allowing healing over 3 to 6 weeks.
Once pain is controlled, gradual return to activity and physiotherapy is essential for recovery.
WHEN IS SURGERY REQUIRED FOR SLIP DISC?
Surgical treatment depends on:
Duration and severity of pain
Response to non-surgical treatment
Presence of neurological symptoms (weakness, numbness)
Bladder or bowel involvement
A lumbar slip disc is a common but treatable condition.
In such cases, early surgical intervention improves the chances of nerve recovery and long-term outcomes.
With early diagnosis and the right treatment approach:
Most patients recover without surgery
Minimally invasive options are available when needed
Long-term outcomes are excellent with proper care
Surgery is usually recommended when:
Symptoms persist beyond 6–12 weeks despite treatment
There is significant nerve compression
Neurological deficits are present
Frequently asked questions
What surgery is advised?
Microdiscectomy: Minimally invasive or key hole surgery.
The surgery is targeted at the disc with minimal handling of the nerves. A procedure that uses a microscope and microsurgical tools to remove the portion of the disc that is pressing against the nerve, relieving the pressure caused by a herniated disc. The aim is remove loose fragments enough to free the nerve and cause relief of pain. The annulus (disc covering) heals naturally allowing normal activity
This procedure is performed either by using a microscope and a tubular retractor or an endoscope. The skin incisions size is between 8mm to 14mm small.
How long will I have to stay in the hospital?
These are day care procedures where the patient can be discharged within 24 hours.
Is bed rest required post surgery?
Post surgery no bed rest is required. The patient is made to walk within 3 hours.
How much disc is removed?
Only the portion of the disc that is herniated is removed. This decompresses the nerve and gives pain relief. The rest of the disc is kept intact. The defect in the disc heals naturally.
What precautions have to be taken?
The surgical wound is covered with a waterproof band-aid. The wound has to be kept dry till it heals (10days). Free forward bending, ground level sitting and lifting of heavy weights(8-10kgs) should be ideally avoided for 3 – 6 weeks. There is no restrictions on walking, travelling or resuming work.
Can there be a recurrence?
The surgery aims to control pain through a keyhole incision. However it does not strengthen or weaken the spine. There is a chance of recurrence if an uncontrolled activity tears the disc. Increasing core muscle strength by exercise is the best protection against a recurrence.
Can I lead normal life after a disc surgery?
Disc surgery does not refrain a person from pursuing a normal lifestyle. However like any other machine, the spine also needs maintenance. For any machine to function optimally the load on the machine (body-weight) should reduce and it should be serviced (core strengthening exercises) regularly.
Is this a safe procedure?
This is safe and effective surgery that allows immediate restoration of activity. The chances of nerve injury are minimized by use of a microscope. The complication rate can be placed at 1% or less.
Dr. Amandeep Gujral is a Senior Consultant Spine Surgeon
He specializes in Minimally Invasive Spine Surgery (MISS) and treats conditions like slip disc, sciatica, neck pain, spine deformity, infections, and tumors.
Providing advanced, patient-focused spine care across Mumbai.
Board certified spine surgeon in Mumbai.
opd@spinecareindia.com
+91-9920966777
© 2025 Spinecareindia.com | Dr. Amandeep Gujral. All Rights Reserved.
The information on this website is for general educational purposes only and is not a substitute for professional medical advice.
